Community Diagnostic Centres
NHS England have announced the creation of community diagnostic centres or CDCs. These are designed to provide additional imaging capacity outside of the traditional hospital model.
PML have been providing these services to the NHS for 16 years and are now part of the NHS England Diagnostic Framework Hub as an accredited provider.
- 140 Dedicated Imaging Centres
- 50+ Commercial Partners
- Specialist Scientists, Doctors & Nurses
- Opthalmology
- Endoscopy
- Patient Satisfaction
- Cost Savings
- Awards & Best Practice
- Growth
- Innovation
Delivering the NHS Long-term plan and boosting out-of-hospital care.
Just before the pandemic struck the NHS had completed a review of diagnostic services called the Richards report, prepared by Sir Mike Richards, the former head of the CQC.
But in a nutshell, we don’t have enough diagnostic equipment, most of it is in hospitals and this leads to problems in operational delivery.
Following on from the Diagnostic review was the GIRFT (Getting it Right First Time) report. In summary, this is about increasing capacity, working more efficiently, innovating and using technology to improve services. A bit like what we do at PML every day.
The NHS Long-Term Plan sets out an ambition to transform capacity and responsiveness of clinical services on a local level. This transformation is at the heart of new models of care and will require closer working and integration across patient pathways.
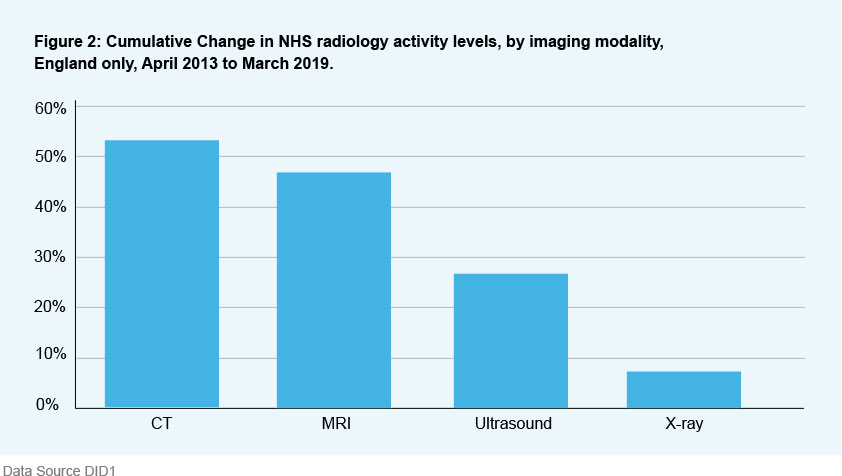
Traditional approaches have been to provide elective diagnostics in acute settings (i.e. hospital-based diagnostics), typically following a pathway from GP referral to hospital consultant, with periods of several weeks between referral to diagnostic tests and additionally further delays between tests and follow up appointments. The diagnostic centres will close that loop, making the patient journey much shorter and more precise.
Community-based diagnostics
Diagnostic tests have been delivered by PML in a community-based setting for the last 16 years, with increased and appropriate use of GP direct access. Joining up primary and specialist follow up care in settings that are closer to patients’ homes is essential if we are to reduce the number of journeys to hospitals, reduce ‘Referral To Treatment’ times and drive efficiency and productivity through constant learning and innovation. For many years, the NHS has suffered a shortfall in equipment and appropriately qualified staff to operate and provide reports to meet the demand. Diagnostic Centres should go a long way to levelling up this capacity and demand mismatch.
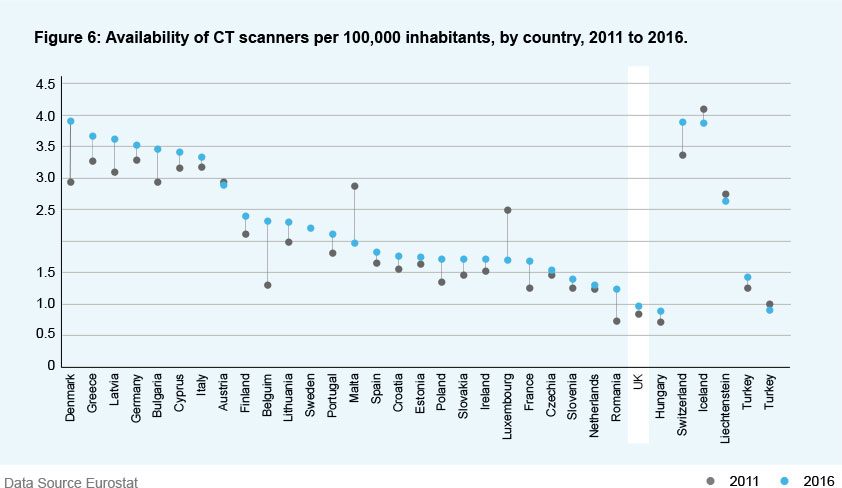
‘Hot & ‘Cold’ sites
Post-pandemic patients will need to feel confident of their safety to re-access care. The separation of elective and non-elective care, with ‘hot’ and ‘cold’ clinical sites, will be part of a future landscape that needs to allow for future waves of pandemics, without compromising on care provision.
PML partner with public and independent sector healthcare providers, equipment manufacturers and other partners to accelerate the growth of community diagnostic centres through providing infrastructure, IT platforms and integrated information systems and create innovative ways of working aimed at improving clinical, experiential, operational and financial outcomes













